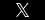My friend Amy Dougherty is a physical therapist in North Carolina and operates Outer Banks Physical Therapy. She is a graduate of the University of North Carolina at Chapel Hill (where I also attended college and law school). She is an outstanding physical therapist and is beloved by her patients on the Outer Banks. Amy answers many of your questions about hip replacement surgery, metal-on-metal artificial hips, and the problems that have arisen from these hip products.
Clay: I want to focus on hip replacement surgery and I know you work with patients who are dealing with that kind of surgery every week. So let me start by asking what are a few reasons a person might need a hip replacement surgery?
Amy: You know, the most common reason is arthritic changes in the hip. So basically arthritis, that is the most common reason. Other reasons can include things like trauma. Some people have congenital mal-alignments where, it is basically called dysplasia where through the process of their development in utero and then following their bony surfaces of the femur, that is the long thigh bone and the acetabulum which is in the pelvis. They do not form correctly, so they might have ill-formed femoral heads. They might have ill-formed or ill-shaped acetabulum. So, the ball and the socket are not really designed well to weight bear. So, a lot of folks that, especially in a young population, that have early onset hip replacements. It is more likely the result of some type of congenital dysplasia. It could be a trauma. So, but arthritic changes is the number one reason and I have total hip replacement patients in my clinic every day. Very popular surgery, yes.
Clay: Very common especially once you get into the middle age and even older.
Amy: Absolutely. It is very common.
Clay: Well, how soon would physical therapy start after a total hip replacement?
Amy: Typically, the PT shows up within 24 hours of your surgery when you are in the hospital. So, what you can expect is basically after you come out of recovery, the physician or the nurse will come and talk with you and tell you when you will start your first PT. Sometimes, it is within 12 hours. It really is all dependent on the amount of time that is projected to be your discharge. Time or day, and that is something that actually frankly is changing dramatically over the course of the last 18 to 24 months. So total hip replacement surgeries are moving from being a two-day event in the hospital, which is what we used to see very commonly, to most likely being a predominantly outpatient surgery within the next five years.
Clay: Outpatient surgery–is that right?
 Amy: That is right, and there is some pretty reasonable science to support why transitioning to outpatient is a great idea and is basically because of infection rates and things like that. And so, they are looking, I mean they being the world of orthopedic surgeons and the world of joint replacement specialist. They are looking to transitioning. It is already happening in some places, not on the Outer Banks, but it is happening in some larger cities where they are doing small groups of folks who are good candidates, so they are essentially very healthy people who frankly do not need to be hospitalized. They can go to an Ambulatory Care Center and safely receive a total hip replacement and go home that same day.
Amy: That is right, and there is some pretty reasonable science to support why transitioning to outpatient is a great idea and is basically because of infection rates and things like that. And so, they are looking, I mean they being the world of orthopedic surgeons and the world of joint replacement specialist. They are looking to transitioning. It is already happening in some places, not on the Outer Banks, but it is happening in some larger cities where they are doing small groups of folks who are good candidates, so they are essentially very healthy people who frankly do not need to be hospitalized. They can go to an Ambulatory Care Center and safely receive a total hip replacement and go home that same day.
Clay: Could it also be maybe that recovering at home is a happier place for people?
Amy: No question. All of us would rather be home than at the hospital, and so the biggest issues that come into play are first and foremost safety, so you have to be safe to go home. Once you are in the recovery room you have to be medically stable. Pain needs to be adequately manage and that is something within the Joint Replacement Community, that is really becoming more and more well-researched and well-managed is how to keep people comfortable while they are recovering from this very big surgery. That is a big event, so managing the pain, making sure that they are safe to ambulate because you can walk on that new hip pretty much as soon as their block wears off as soon as anesthesia allows.
Clay: So whenever you come home, whether it is the same day or a couple days later and the patient is able to get to your office, how soon– so walk us through what PT might look like in the first visit to your office and then in the weeks that follow.
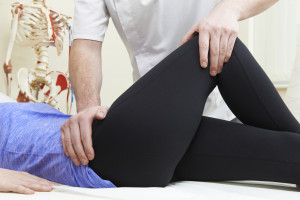
Amy: Typically, I will sometimes see people that are coming straight from the O.R. Basically, they may spend a day and a night in the hospital they come home and they are usually starting with me within a day or two of being home. So sometimes I will see them immediately post-op, some surgeons want those patients to be seen at home anywhere from two to four weeks. Generally based on surgeon preference. Sometimes it has to do with family logistics in that patient might live alone. They can not drive those first couple of weeks. So there are some issues that play into the decision making on whether they start outpatient, which is my clinic, or whether there is seen at home for home-based physical therapy. But if you come to my clinic the first thing that is going to happen is you are going to undergo an assessment, and that is basically where after doing a bunch of intake paperwork, where we make sure that you are actually medically stable, we start talking about your function. We start talking about “Hey, how are you doing?” What is your pain like?” We use pain scales and I expect because it has become such a big movement in orthopedics to better manage people’s pain so that they move.
Because we know that one of the things that is most helpful after joint replacement surgery, be at a hip or knee, is the ability to move. If you have got so much pain, you can not move all of a sudden, your risk factors go up substantially in regards to blood clot or onset of pneumonia. So, we know that moving is important. We will talk about your pain. Make sure that your pain is being adequately managed and then we will start looking at that lower extremity. I will have you walk for me. I will look at edema, will look at bruising, depending on whether your surgical dressings are off or not. I will look at the surgery site. Make sure it all looks good clean and dry, occlusive bandages or it should be in place at that point and then, just basically initiate the onset of PT which is assessing, and then addressing strength loss this most in deficits. We spend a lot of time talking about precautions, because there are some precautions after hip replacements depending on the approach that the surgeon has taken. So, there are some options available in regards to whether you have what is called an anterior approach or posterolateral approach. And so, there are some precautions and we make sure that the patient is well versed in that, and understands why the precautions are important. And then, we start to exercise, we start to move.
Clay: I know it is different for different patients based on how fit they might be, how young they might be. But how long does that therapy last working with you? And then when do you say “Okay, you are free to go but take these exercises home with you and make sure you do them”?
Amy: We start immediately. We start the first day they are there. Nobody leaves my clinic without having things to work on at home.
Clay: And so how long do those exercises last with you versus when you say “Okay you are released from me and you can do these at home without me”?
Amy: Frankly, it depends, and what I have come to realize through a lot of years of clinical practice is the fitness level that someone takes into the operating room. Absolutely dramatically affects how long they are with me. So, if you are pretty active, pretty strong, pretty fit, you just have a bad hip, and you can be all those things by the way, and still have a bad hip. So if you are pretty mobile and you have maintained pretty decent strength pre-op, you are not going to spend much time with me. A couple weeks, maybe. If you are really debilitated and we see this very commonly in people who have really put off having the joint replacement, maybe waited a lot longer than they should have.
Sometimes, there is a concomitant problems going on at the knee, at the foot and ankle, on the contralateral side, will see some problems that affect their ability to ambulate. And at the end of the day, with a hip replacement, our goal is generally normalize gait. I mean, that is what we are looking for and everything that normalized gait entails and so that strength, mobility, balance, neuromuscular control of the extremity. So at the end of the day, that is really what we are looking for is normal gait.
 That is what frankly people that are having their hips replaced, they will tell you “I can not walk. I can not ascend or descend the stairs.” I live at the beach, you know people’s inability to get onto the beach is a huge issue. So because you take gait, and now you put it on an unstable surface like sand and the demands are exceptionally greater to be able to walk the beach than are to walk on the sand. So that is something in that first visit that we talk about “What are your goals?” I will specifically ask the patient when I am interviewing them, when I am evaluating them “What are your goals?” [and] “What is it that you have this hip replacement for a reason?” [and] “It is an optional surgery. Your life did not depend on you getting a hip replacement. So, what are your goals?”, “What did you decide, you have decided to make this commitment of time, money, risk, you have done those things to do something. Is it to be able to get through the night without pain?” For some people, that is their ultimate goal. Most people, it is mobility. I want to be able to get onto the beach, you know, some people I work in a beach community. I have patients that their goal is: I need to get back on my surfboard.
That is what frankly people that are having their hips replaced, they will tell you “I can not walk. I can not ascend or descend the stairs.” I live at the beach, you know people’s inability to get onto the beach is a huge issue. So because you take gait, and now you put it on an unstable surface like sand and the demands are exceptionally greater to be able to walk the beach than are to walk on the sand. So that is something in that first visit that we talk about “What are your goals?” I will specifically ask the patient when I am interviewing them, when I am evaluating them “What are your goals?” [and] “What is it that you have this hip replacement for a reason?” [and] “It is an optional surgery. Your life did not depend on you getting a hip replacement. So, what are your goals?”, “What did you decide, you have decided to make this commitment of time, money, risk, you have done those things to do something. Is it to be able to get through the night without pain?” For some people, that is their ultimate goal. Most people, it is mobility. I want to be able to get onto the beach, you know, some people I work in a beach community. I have patients that their goal is: I need to get back on my surfboard.
Clay: Right.
Amy: If it is somebody who basically just wants to be able to grocery shop and, be able to get their groceries in and out of their car independently and walk with a normal gait, unless they are profoundly weak when we start, it is not going to be too long. So, I know that is a ridiculously vague answer.
Clay: No, everybody’s different.
Amy: But fundamentally, everybody’s different with what they bring into the operating room and everybody’s different with their expectations following. So, the way I rehab a 35 year old, and the expectations and the demands that 35 year old is going to place on that new hip is going to be profoundly different than my 82 year old.
In Part 2, Amy and I discuss recovering from hip replacement surgery, returning to activity and even sports after hip surgery, and the importance of getting active and staying active.
 North Carolina Product Liability Lawyer Blog
North Carolina Product Liability Lawyer Blog