Today I will discuss the Camp Lejeune toxic water litigation, and if there is one fact that I can leave you with in this post, it is this: the deadline for bringing an administrative claim is August 10, 2024.
Today I will discuss the Camp Lejeune toxic water litigation, and if there is one fact that I can leave you with in this post, it is this: the deadline for bringing an administrative claim is August 10, 2024.
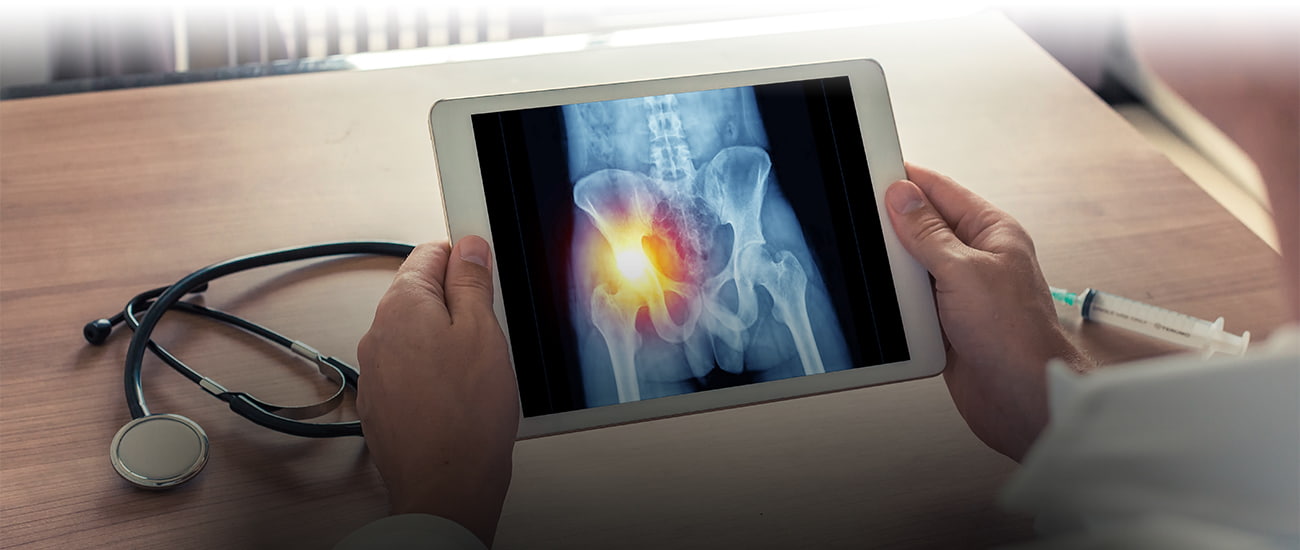
The Camp Lejeune legislation that was passed about two years ago is rather extraordinary, and what it has done is allowed people who were injured years and sometimes decades ago to bring a current viable claim against the federal government for serious illness and injury suffered as a result of toxic water in and around the Camp Lejeune Marine Corps Base, but if you have a claim and do not file an administrative claim with the US Navy by August 10, 2024, then you will be out of luck, and you will have no recourse to compensation.
Now the good news is filing the administrative claim, which starts the ball rolling to identify to the federal government that you want to bring a claim, filing that administrative claim is somewhat straightforward. I do not believe individuals should represent themselves in this matter. I believe you need an attorney who’s familiar with this litigation to handle that process for you, but the good news is the administrative claims process is not nearly as complex as actually filing a lawsuit, which you certainly will have to do in the months after you file an administrative claim, so write down the date, put it on a Post-it note, or tape it to your refrigerator; and you need to contact an attorney immediately if you believe you or someone you loved, even a deceased parent, or even a grandparent, may have been harmed by exposure to the toxic water at Camp Lejeune.
 North Carolina Product Liability Lawyer Blog
North Carolina Product Liability Lawyer Blog